INTRODUCTION
Ovulation induction has been one of the most significant advances in the treatment of infertility. Although considered routine today, its origins date back only a relatively short time. In 1909, Crowe and associates demonstrated that partial hypophysectomy of adult dogs promoted atrophy of the reproductive organs.1 When the same experiment was performed on juvenile animals, they failed to achieve sexual development.
However, it required two more decades for investigators to establish that the reproductive systems of the male and female are under control of the pituitary gland. These independent and almost simultaneous discoveries by Zondek and Ascheim2 and Smith and Engle3 paved the way for the use of gonadotropins in clinical medicine. Serum gonadotropins from pregnant mares were soon isolated, extracted, and used successfully for ovulation induction. Unfortunately, use never became widespread because of the high degree of antigenicity.4
Subsequently, gonadotropins were extracted from the human pituitary glands that contained both follicle-stimulating hormone (FSH) and luteinizing hormone (LH).5 However, their use was limited by the small number of pituitary glands available for extraction purposes.
By the early 1960s, common techniques for extracting gonadotropins from the urine of menopausal women (human menopausal gonadotropins [hMG]) were developed, thus providing a plentiful source of this substance.6 The clinical trials by Lunenfeld and colleagues7 in 1962 resulted in the successful induction of ovulation and pregnancy using hMG (Pergonal; Serono Laboratories, Randolph, MA) in combination with human chorionic gonadotropins (hCG).
At that time, the only clinical parameters for monitoring patients were cervical mucus changes and pelvic examination. The end result was a high percentage of ovarian hyperstimulation. The subsequent introduction of estrogen monitoring and ultrasonography added safety and effectiveness, thus allowing ovulation induction to enter the modern era.8 Urinary gonadotropins have also been available from Organon and Ferring Pharmaceuticals (Menopur) for 40 years.
The techniques involved in gonadotropin production originated in 1954, using kaolin extracts from pooled menopausal urine. These preparations contained FSH and LH activity in comparable amounts and provided a relatively unlimited source of gonadotropins. Although one pituitary gland contained as much FSH as 2–5 L of postmenopausal urine, the identification of Creuzfeldt-Jakob disease resulted in the banning of pituitary compounds from clinical use.9
The demand for urinary gonadotropin has increased steadily, resulting in temporary shortages of urinary gonadotropins. This is understandable in view of the fact that in 1996, the population size of women between 19 and 34 years in the developed world was estimated to be in excess of 135 million.
Using an estimate of 8% infertility, the pool of the infertile population would exceed 10 million, resulting in 700,000 new patients entering this pool every year for the immediate future. This requires more than 100 million liters of urine to be processed. Up to 1997, more than one million women had been treated with these urinary products.10
To accommodate the increasing demands for the gonadotropins, producers of these products have developed recombinant technologies. Human recombinant FSH has been produced in Chinese hamster ovary (CHO) cells by Ares-Serono (Gonal-F; Geneva, Switzerland).11
Genes encoding the a-FSH and b-FSH subunits have been isolated from a gene bank and the functional genes introduced into the genome of the CHO cell line. The selected recombinant cells synthesize both subunits of FSH and secrete glycosylated bioactive dimeric FSH. The medium is harvested and the FSH is purified, initially by immunochromatography with a specific anti-FSH monoclonal antibody and later by further purification steps. The final product has a specific activity of more than 10,000 internation units of FSH per milligram of protein. CHO cells have also been used to develop recombinant FSH by Organon (Follistim, West Orange, NJ, USA).
In addition to the recombinant technology for developing the gonadotropins, Ares-Serono has developed a highly purified urinary FSH preparation, Fertinex. It has higher specific activity and far fewer impurities than any of the nonrecombinant preparations, thus allowing it to be administered subcutaneously with reduced potential for adverse reaction at the injection site. In contrast to Metrodin, which was removed from the market with the introduction of Fertinex, the purification process for making Fertinex involves capture of FSH proteins by monoclonal antibody and a number of high-performance liquid chromatography steps to remove non-FSH proteins.
The result is an FSH preparation virtually devoid of LH that has a specific activity of 9,000 international units FSH per milligram of protein. The terminal half-life of Fertinex HP is 39–45 hours, depending on the mode of injection. This half-life is approximately twice that of Metrodin. Most of the FSH in use today is of the recombinant variety.
While gonadotropins remain the mainstay of ovulation induction, recent studies evaluating the role of dietary factors such as a micronutrient with a positive effect on ovulation may in the future influence gonadotropin need and dosages. In a study of 438 women over an 8-year period, using a multivitamin at least three times per week was associated with a reduced risk of ovulatory infertility.12 The long-term impact of vitamins on ovulatory infertility requires further elucidation.
STRUCTURE AND PHARMACOLOGY
Gonadotropins are glycoproteins with an approximate molecular weight of 30,000 daltons. They consist of approximately 20% carbohydrates (Table 1). They are heterodimers composed of two subunits, a hormone-nonspecific α subunit and a hormone-specific β subunit.
These subunits are not covalently linked, but are held together through a portion of subunit called a seatbelt that wraps around the α subunit. This seatbelt region is primarily responsible for the influence of subunit or receptor binding specificity.12
Table 1. Primary structure of LH, FSH, and hCG
| Hormone | Molecular Weight | Amino Acid | Sialic Acid Carbohydrate Residues | Half-Life in Circulation |
| LH | 28,000 | 1–2 | 50 min | |
| α | 089 | 2 | ||
| β | 115 | 2 | ||
| FSH | 34,000 | 5 | 3–4 h | |
| α | 092 | 2 | ||
| β | 111 | 2 | ||
| hCG | 38,000 | 20 | 6–8 h | |
| α | 089 | 2 | ||
| β | 145 | 6 |
LH, luteinizing hormone; FSH, follicle-stimulating hormone; hCG, human chorionic gonadotropin.
The sialic acid content varies among the vital proteins and accounts for the differences in half-life. hCG has 20 residues, FSH five, and LH one or two. The greater the sialic acid content, the longer the biologic half-life. The function of the carbohydrate groups is not fully known.
However, it is known that removal of the terminal neuraminic acid (sialic acid) residues greatly shortens the circulating half-life of that hormone in the blood. All the gonadotropins, and thyroid-stimulating hormone as well, share a common a subunit of approximately 92 amino acid residues in the same sequence. In contrast, the β subunits of FSH, LH, and hCG are specific for each hormone and are responsible for their biologic specificity. The gene structures for both the α and β subunits are known, and a single gene type apparently is responsible for coding all α and β subunits within the species.13
Synthesis begins with the transcription of the gene in the nucleus. Several upstream regulatory elements in the genes mediate cyclonucleotide, steroid, and gonadotropin-releasing hormone (GnRH) control of the gonadotropin gene expression. After transcription, capping, intron splicing, and polyadenylation, the messenger RNA for both subunits is transported to the site in the cytoplasm where it is translated.
Several species of FSH are present in the pituitary gland and serum.14 The principle difference among these species is the terminal position of the carbohydrate residues, which affects the acidity, receptor-binding affinity, and, most importantly, half-life and biologic activity.15, 16
The presence of estrogen results in pituitary secretion of FSH with a lower sialic acid content.15, 17 For this reason, men and postmenopausal women secrete FSH with a high sialic content and longer half-life and less biologic activity than the less acidic forms present in premenopausal women or estrogen-treated men.18
New data are being established on the pharmacokinetics of FSH.19, 20, 21, 22 The total clearance of recombinant FSH (0.15 L/h) is comparable with that of urinary FSH (0.5 L/h) as determined by immunoassay and bioassay data. The two preparations also have similar initial and terminal half-lives (2 and 17 hours, respectively). For this reason, both recombinant FSH and urinary FSH protocols can follow comparable treatment regimens.
PHYSIOLOGY
Each month in the normal menstrual cycle, a large cohort of follicles initiate development. This follicular development up to the antral stage appears to be gonadotropin-independent.23
However, it has been suggested that development of a primordial follicle (an oocyte surrounded by a single layer of granulosa cells) into an antral follicle that is capable of responding to gonadotropins may require 10 weeks. Only 0.1–0.5% of the total follicle population is in some degree of growth; the others are resting primordial follicles.24 FSH receptors do not appear until the transition of these granulosa cells or until the autodifferentiation of these granulosa cells into cuboidal shapes. The absolute number of FSH receptors per granulosa cell does not increase beyond this early stage of follicular growth.
Receptors for estradiol, progesterone, and testosterone appear as the follicle develops during the late secondary and early tertiary stages. From this point on, further development requires FSH. From the several hundred primordial follicles that initiate growth each month, no more than 20 precursor follicles are likely to be present at the beginning of the menstrual cycle.
The sequence of events that occurs over the ensuing 2 weeks is well delineated. However, the absolute criteria for the selection of a single follicle as dominant over the rest of the cohort remain elusive. Because the dominant follicle is enriched with FSH receptors, it continues growing despite decreasing FSH levels.
cAMP binds to a regulatory subunit of protein, resulting in the phosphorylation of regulatory proteins that stimulate gene transcription and translation to encode P450arom, 17b-hydroxysteroid dehydrogenase, P450scc, 3b-hydroxysteroid dehydrogenase, and LH receptor.25, 26
Other factors that contribute to follicular growth such as insulin-like growth factor 1, fibroblast growth factor, and epidermal growth factor amplify FSH stimulation of meiosis. Estrogen also contributes to FSH amplification by enhancing FSH-stimulating cAMP and cAMP-dependent protein kinase. Thus, granulosa cells achieve maximal response to minimal concentrations of FSH. However, FSH is detectable in follicle fluid only when the androgen-to-estrogen ratio exceeds 1.27
Therefore, conditions such as polycystic ovary syndrome in which androgen levels predominate result in markedly reduced exposure of granulosa cells to FSH.
As the follicle develops, it secretes, among other things, low levels of estrogen and inhibin that further reduce pituitary FSH production. The appearance of LH receptors on granulosa cells of preovulatory follicles is accompanied by the reduction of FSH receptors, reduced intracellular cAMP levels, and resultant follicle degeneration. Although exogenous FSH stimulation may be saving follicles from degeneration, the saved follicles may not be capable of either fertilization or implantation.
In a time-dependent and dose-dependent regimen, FSH induces an aromatase enzyme. This enzyme converts the ovarian stroma androgen production induced by LH into estrogens. When the critical level of estradiol is reached, the pituitary gland responds paradoxically with a gonadotropin surge of LH that initiates resumption of meiosis and follicle rupture.28 The protein gene c-mos has been identified in eggs in relatively high concentrations. The role of c-mos appears to be that of blocking the degradation of cyclin, a protein responsible for maintaining metaphase II arrest.
Studies suggest that the LH surge causes germinal breakdown and completion of metaphase II by reducing intracytoplasmic levels of c-mos.29 Therefore, LH functions to overcome the inhibition that prevents resumption of meiosis and maturation.
In disorders that affect menstrual regularity, the dynamic interactive chain of events between the hypothalamus, pituitary, and ovary is perturbed. Patients with hypothalamic anovulation have a relative deficiency of both FSH and LH. In polycystic ovary syndrome, the production of LH relative to FSH is excessive.
The accompanying increased LH-to-FSH ratio results in the production of elevated androgen levels from the ovarian stroma that cannot be aromatized to estradiol by an immature cohort of developing follicles. These excess ovarian androgens, in concert with adrenal androgens, are mostly aromatized to weak estrogens in the adipose tissues, an event that further inhibits pituitary increases of FSH. The result is a self-perpetuating cycle leading to the clinical symptoms of obesity, hirsutism, and anovulation with subsequent infertility.
More recently, studies in women who are normal in weight and cycle length and who do not have a history of an eating disorder have been found to have abnormal associations between leptin, LH pulsatility, and metabolic rate.30 As more is learned about this underlying pathophysiology, alternative and more selective approaches to ovulation induction may evolve.
SELECTION OF PATIENTS FOR GONADOTROPIN THERAPY
The use of gonadotropins has expanded tremendously since their introduction into clinical medicine more than 40 years ago. The initial indication for administering gonadotropins was hypothalamic–pituitary insufficiency. These patients typically are amenorrheic and do not have withdrawal vaginal bleeding after a progesterone challenge test.
One must exclude uterine causes of amenorrhea such as congenital abnormalities or severe uterine adhesions that occur with Asherman’s syndrome. The presence of low or normal FSH levels excludes ovarian failure and points to pituitary insufficiency. Although pulsatile GnRH could be used as an alternative treatment to gonadotropins unless the patient has a pituitary stalk transection, gonadotropins are overwhelmingly the treatment of choice.
The second group of patients who frequently receive ovulation induction with gonadotropins are those with hypothalamic–pituitary dysfunction with normoprolactinemia and normal androgen levels. Such patients typically are classified under the category of luteal phase defects, but they may also present with amenorrhea. Such patients usually experience withdrawal bleeding after the administration of progesterone.
Common circumstances that lead to this type of hypothalamic dysfunction include stress, extreme changes in body weight, or excessive athletic activity. Although clomiphene citrate is typically administered as the first line of treatment, women who do not respond with dosages of up to 150 mg per day for 5 days or who do not conceive after three to six cycles of clomiphene therapy should become candidates for gonadotropin treatment.
Iatrogenic cervical factor is another indication for gonadotropin treatment. In such instances, a well-timed postcoital test is poor and a lack of cervical secretions results in an inability for sperm to gain passage into the female genital tract. This may be caused by previous cautery of the cervix, an extremely large conization of the cervix, or by an antiestrogen effect of clomiphene citrate.
One can consider administration of estrogen in low dosages such as ethinyl estradiol 20 μg or a conjugated estrogen such as Premarin (Wyeth-Ayerst Laboratories, New York, NY, USA) 0.3 mg daily on cycle days 10–17. Should administration of estrogen fail to achieve adequate cervical mucus secretions, then either FSH or hMG combined with hCG should be considered as an alternative treatment combined with intrauterine insemination (IUI).
Gonadotropins are also administered to hyperandrogenic women with hypothalamic–pituitary dysfunction. This type of patient might be classified as the polycystic ovary patient. A typical history includes acne, seborrhea, and hirsutism commonly associated with obesity.
These patients commonly have androgen levels at the upper limits of normal, and approximately one-third display an increased LH-to-FSH ratio.31 An ultrasound examination of the ovaries often reveals multiple follicles on both ovaries. If the patient has a BMI of 30 or more, weight loss should be encouraged as the first line of treatment.32 Increasingly, these types of patients are being offered treatment with oral hypoglycemic agents such as the biguanide metformin either alone or in combination with clomiphene citrate before using gonadotropins.
This is particularly likely in patients who are insulin-resistant with acanthosis nigricans and who have a body mass index (BMI) greater than 27 kg/m2.33 Increasingly, the oral non-steroidal aromatase inhibitor letrozole is being used for ovulation induction for PCO patients who fail clomiphene citrate.34
Although gonadotropins were intended for women who are anovulatory or who have significant hypothalamic–pituitary dysfunction, gonadotropins are also used for presumably ovulatory women. Such treatment is not without controversy. It is performed primarily for women with unexplained infertility in whom it is believed that the combination of gonadotropins with IUI will improve fecundity and perhaps shorten the window of time required to achieve conception.35
This empiric use of hMG is associated with a pregnancy rate of approximately 12%. Such rates must always be compared with background success rates of untreated women with unexplained infertility. The empiric use of gonadotropins must be presented to patients as being of uncertain value. In addition, new information suggests that women’s cycles may not be as regular as reported. In a study of 65 healthy fertile women aged 19–44 (mean 33.5 years) studied for more than 515 cycles with daily collection of urine for measurement of LH, FSH, estrogen (estrone 3 glucuronide, [E1G]), and progesterone (pregnanediol 3 glucuronide, [PdG]), the results showed tremendous variation.
Although the mean overall cycle length was 28.4 days, the range was 14–50 days36 (Table 2). Similarly, there was significant variation from month to month both between individuals and within the same individuals (Table 3).
Table 2. Parameters of cycle duration (days)
| Interval | Mean | SD | Range |
| Overall cycle length | 28.4 | 3.7 | 14–50 |
| Follicular phase length | 15.0 | 3.7 | 04–35 |
| Luteal phase length | 13.5 | 1.7 | 07–20 |
Table 3. Interindividual and intraindividual variability
| Mean | Between Individuals | Within Individuals | |
| Follicular phase length | 15.4 | 08.5 | 8.9 |
| Mean initial FSH (U/L) | 05.6 | 12.6 | 5.3 |
This extreme variability among so-called normally cycling women appears to represent an undiagnosed cause of reduced fecundity and suggests that in this group of women, before ovulation induction, one should consider careful monitoring of the cycle either in the office or at home with an over-the-counter Clear Blue Fertility Monitor that is capable of monitoring both E1G and PdG in the home setting and offers patients a clear understanding of their menstrual cycle reality and a 5-day window of fertility, capturing both the estrogen and LH increase.
PRINCIPLES OF OVULATION INDUCTION
Although there is considerable variation in the actual use of gonadotropins for ovulation induction, several principles are important if one is to optimize success rates and minimize complications. In contrast to in vitro fertilization, in which the general intent is to mature large numbers of follicles in synchrony, the primary goal of ovulation induction is to encourage the recruitment, maturation, and development of only one or two preovulatory follicles. FSH appears necessary in the early phases of the cycle to recruit and select these follicles.
For growth and maturation, both FSH and LH are necessary. Women who produce endogenous LH are likely to respond comparably well to either purified FSH or preparations that contain both LH and FSH.37 Therefore, an increasing tendency has been for either hMG or purified FSH preparations to be used with comparable expectations.
Although no one set protocol is considered preferential over another, certain principles generally apply. Ovulation induction should be viewed as the follicular phase of the cycle; therefore, ovarian stimulation should be anticipated to require 6–14 days. Stimulations in which less than 6 days of medication are administered generally yield poor results.
Likewise, stimulations requiring more than 2 weeks often result in failure. In general, 5 days of 75–150 IU/day (1 or 2 ampules of Pergonal, Humegon, Fertinex, or recombinant FSH) is the optimal way to begin, followed by measurements of serum estradiol and ultrasound examinations to monitor follicular growth and development and to ensure safety. Follow-up scans should be scheduled every other day or every day, as clinically indicated. An example of an approach to ovulation induction is shown in Figure 1.
Both ultrasound and estradiol assessment are needed for safe and effective monitoring of ovulation induction. Failure to use both greatly increases the risk of ovarian hyperstimulation and multiple births.38
|
|
If no increase in estradiol occurs on the morning of the fifth day of stimulation and there is no evidence of alarming clinical signs, the daily dosage of gonadotropin may be increased by one or two ampules daily; however, no rule prevents one-half an ampule of gonadotropin from being added if deemed clinically appropriate. That dosage is then continued for an approximate additional 4 days to allow time for follicle growth and maturation.
Once an effective dose is established, as determined by a clinically significant and steady increase in estrogen values and follicle growth, further increments of the gonadotropin are neither warranted nor indicated. Estradiol increases that exceed 100% daily are excessive and may forecast ovarian hyperstimulation. Should this occur, the dosage should be reduced by 1 ampule daily. If the estradiol level does not increase steadily, the daily dosage should again be increased by 1 or 2 ampules for an additional duration of approximately 4 days.
The ideal estradiol level to trigger hCG is approximately 450–900 pg/mL (1650–3300 pmol/L) and one or two follicles with a diameter of at least 16 mm at an endometrial thickness of 8 mm or more. Serum progesterone assessment is also useful to be sure there is no premature luteinization. Ideally, the progesterone level should be less than 1 ng/mL (3 nmol/L). At that point, ovulation is triggered by the administration of 5000–10,000 international units of hCG.
Patients with a polycystic ovary presentation have an increased tendency to hyper-respond to gonadotropin treatment. For this reason, I have developed a protocol that uses a much lower gonadotropin dose for a longer duration of time (Fig. 2).39
Others such as Steve Frank and Howard Jacobs in London advocate similar protocols. Further modifications of this low dose approach have been adapted for use with PCO patients undergoing in vitro fertilitzation.40
|
|
INFORMED CONSENT FOR OVULATION INDUCTION
Because of the widespread use of gonadotropins, the potential for seeing a significant adverse effect within one’s professional career is increased. In addition, it is becoming increasingly common for groups of physicians to work together either in one practice or in satellite offices in which care of patients and the responsibility for them are shared.
As a result of this increased usage and of the fragmentation of care, informed consent has become increasingly important.41
Ovulation induction should rightfully be viewed as a safe and reasonable form of treatment for widespread application. However, serious side effects or serious complications do uncommonly occur. In view of this fact, and because our patient base consists largely of healthy young women, the treating physician must realize that complications can and do arise, and this information should be shared with patients and documented in the record.
On-call coverage must be knowledgeable and available daily. Endocrine laboratory results and ultrasound capabilities should also be available daily or certainly almost every day, and the results must be reviewed and interpreted each day to prevent potentially serious side effects. To help ensure that this occurs, I have developed a consent form to summarize the information provided to patients before ovulation induction (Figs. 3 and 4).
|
|
|
|
The potential side effects are reviewed carefully with the patient and ideally with her partner before initiating treatment. With increasing numbers of patients self-administering medications, it is our responsibility to provide simple instructions concerning injections.
This is necessary to prevent the injection from being administered too low on the buttocks, which could increase the risk of sticking the sciatic nerve or a large blood vessel. Careful documentation of the instructions should be written in the chart. If the physician or nurse at the office administers the injection, it is very useful to make a notation on which side the injection was administered and the location (e.g., identify the upper outer quadrant of the left buttock). This type of documentation is particularly helpful if a problem associated with a particular site is involved and the medical record clearly states that the injection was administered elsewhere.
Patients must be informed that there is approximately a 20% risk of multiple births with these medications, three quarters of which are twins. However, patients must also be advised that higher-order pregnancies are not rare, and there may be as many offspring as there are developing follicles. Over the past decade, the number of twins and higher order multiple births attributed to in vitro fertilization has steadily reduced, while the total number of multiple births has not declined.42
If more than three follicles are present before the administration of hCG, the follicle number can be reduced by follicle aspiration (if the goal is simply to lower the number of possible offspring) or in a procedure setting (if the goal is to perform in vitro fertilization followed by cryopreservation). Selective reduction of the gestational sacs can also be performed if the number of pregnancies exceeds three.
However, it goes without saying that it is preferable to prevent the higher-order pregnancy that places the patient at risk for losing all her pregnancies than to undergo a selective reduction on both a clinical and bioetical basis. Because these alternatives may be unacceptable to some patients, a frank discussion should be included before treatment to monitor her cycle appropriately.
Patients must be warned of ovarian hyperstimulation; some degree of ovarian enlargement occurs in most patients and mild ovarian hyperstimulation occurs in more than 40% of patients.43 Symptoms consist of mild bloating without ascites and ovarian diameters of 5 and 7 cm. In moderate ovarian hyperstimulation, the ovaries enlarge to 7–10 cm in diameter with an increase in abdominal girth, bloating, and abdominal discomfort. An ovarian diameter of more than 10 cm is considered severe; it occurs in approximately 1% of patients and is accompanied by a number of typical symptoms (Table 4).
The peak ovarian size usually occurs approximately 10 days after the ovulatory dose of hCG, and this is an excellent time to ask the patient to return for a follow-up visit. Patients whose ovaries contain ten or more follicles per side at the time of hCG are most likely to have severe ovarian hyperstimulation.
Table 4. When to call your physician
| Weight gain >3 lb in 1 day |
| Shortness of breath |
| Abdominal pain |
| Chest pain |
| Pants become tight |
| Unable to stand upright |
| Dizziness |
| Calf pain |
| Arm or leg weakness |
An adnexal diameter of 10 cm or more in the presence of ascites constitutes ovarian hyperstimulation syndrome. Its pathophysiologic basis stems primarily from increased capillary permeability mediated by the ovarian renin–angiotensin cascade, histamine, serotonin, vascular endothelial growth factor, cytokines, and vasoactive endothelial substances.44, 45, 46, 47
Other potential side effects associated with this syndrome include pleural effusion and an increased risk of thrombosis as a result of hemoconcentration, a sludging of the blood flow through the arteries. This latter event appears to be occurring more often, primarily because of the increased numbers of patients exposed to gonadotropins annually. Ovarian hyperstimulation or ovarian hyperstimulation syndrome should be viewed as a potentially life-threatening problem.
Treatment of ovarian hyperstimulation syndrome can usually be achieved conservatively through hospitalization. The patient should be monitored for input and urinary output. Fluid replacement should be accomplished with normal saline or lactated Ringer’s solution, because a hypotonic solution may increase third spacing. Daily weights are helpful to assess fluid retention.
A weight gain of more than 3 lb/day may require treatment. This is usually not achieved with diuretics, which lead to further hemoconcentration, but rather with hypertonic solutions such as albumin or dextran to draw third-spaced fluid back into the vascular tree. Paracentesis or culdocentesis of the ascitic fluid can lead to dramatic improvements,48 but this latter approach is rarely necessary. The number of examinations should be limited to reduce the risk of ovarian rupture. Abdominal girths measured daily with a tape measure allow objective quantifying of size. Daily blood tests for hematocrit and electrolytes provide a basis for assessing the degree of hemoconcentration and electrolyte imbalance.
Rarely, the enlarged ovary undergoes torsion; this is a surgical emergency. Although oophorectomy was once advocated as the only treatment, it is now known that the ovary can be untorsioned and retained without oophorectomy. Doing so does not increase the risk of thrombosis or embolus.
The final short-term complications of gonadotropin therapy are related to pulmonary embolus, stroke, and death. These events are not limited to patients who have pre-hCG estradiol levels exceeding 2000 pg/mL; I am aware of cases of cerebrovascular accidents in which the estradiol value was less than 1000 pg/mL at the time of hCG administration.49
Although complications can be prevented with high probability, they cannot be prevented with absolute certainty, even if one is cautious. For this reason, all patients must be made aware of the potential risks of gonadotropin therapy, and the conversation must be documented in the chart.
The final area of informed consent involves the long-term risks of gonadotropin therapy. A study published in 1992 suggested that fertility drugs may cause ovarian cancer.50 In that report, however, only ovarian cancer patients were studied. Of 620 women with ovarian cancer, 3% reportedly had taken fertility drugs, compared with only 1% of 1000 noncancer controls.
The findings in this study were based on only 31 women who had used infertility medications. The study failed to report what dosage of the fertility drugs the women had used, how long they received the medications, or what drugs were used. The study did suggest that pregnancy, breastfeeding, and oral contraceptive use may decrease a woman’s chance of ovarian cancer. These latter epidemiologic data are in accord with the current information relevant to ovarian cancer. Subsequent studies have been performed retrospectively looking at women who received gonadotropins. The bulk of the evidence available today suggests that women who have infertility have an increased risk of ovarian cancer over those who are fertile.
However, infertile women who use ovulation-inducing agents do not appear to be at increased risk of ovarian cancer over women who do not conceive and who do not take fertility drugs.51 Therefore, based on the results of these data, patients must be advised as to the potential risks that exist but reassured that the medications appear to add little to the risk over and above that of the infertility per se. Even so, most infertility patients appear willing to tolerate a slightly increased risk of ovarian cancer, if such a risk were the case.52
Although no amount of preparation, information, or careful monitoring can eliminate all complications and side effects, patient education is time well spent. Not only will she and her partner be less likely to be angry if a complication occurs but also will she also be able to notify the physician before a problem becomes serious.
RESULTS OF TREATMENT
Results of treatment have been compiled for approximately 8000 anovulatory patients who received hMG for more than 22,000 cycles, in more than 1000 ovulatory cycles in which hMG was used in combination with IUI, and in nearly 140,000 cycles stimulated with gonadotropins for assisted reproductive technology.31 The conception rate based on these data for anovulatory cycles is 11.7% per cycle and 34.2% per patient.
Success rates for ovulatory women undergoing hMG stimulation in conjunction with IUI approach 13% per cycle, and 26% per patient. Similar results are achieved with assisted reproductive technology.
Patients with amenorrhea caused by hypothalamic–pituitary insufficiency or failure achieve pregnancy at a much higher rate, with results approaching 80%. When one divides the success rates by age, those younger than age 35 achieve more than a 95% success rates after six treatments.
Patients older than age 35 achieve a pregnancy rate of approximately 60%. Patients who are oligo-ovulatory and who do not achieve success with clomiphene citrate can anticipate success rates of approximately 55%. Once again, age plays a major role. Patients older than age 35 are much less likely to achieve pregnancy than those younger than age 35. Patients with polycystic ovaries, in general, achieve ovulation in more than two thirds of cycles; however, only one third of patients ultimately conceive within 6 months.33
It will be interesting to see if the oral hypoglycemic agents and aromatase inhibitors increase conception among this group of patients and whether their miscarriage rate decreases. The anticipated miscarriage rate after gonadotropin treatment is slightly more than 20%.53 There appear to be no significantly increased risks of congenital abnormalities or abnormal development among treated mothers and their offspring.54 When patients are found to be poor responders to ovulatory stimulating medications, altering the individual amounts of LH and FSH appears to produce no further benefit.55
CONCLUSION
Ovulation induction with gonadotropins has become a standard part of the armamentaria of physicians treating women with ovulatory dysfunction. The treatment has been used effectively for more than 50 years. Urinary preparations of gonadotropins are being superseded by recombinant technology; this increases the consistency of the medication, possibly will improve outcomes,56 and, one hopes, decrease the cost.
As a result, we can continue to view ovulation induction as a major and ever-improving component in the treatment of infertility.
Author
Machelle M. Seibel, MD
Professor of Clinical Obstetrics and Gynecology, University of Massachusetts School of Medicine, Worcester, Massachusetts, USA

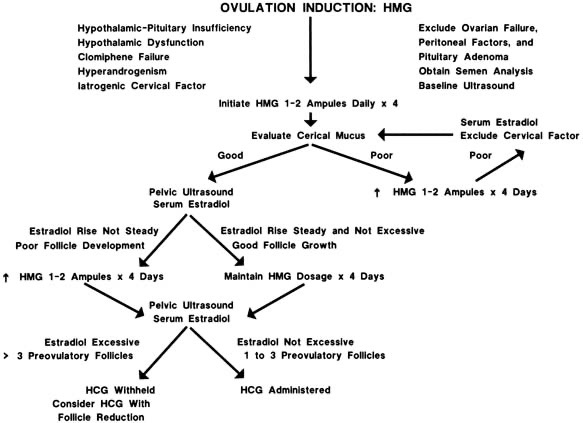 Fig. 1. Ovulation induction with hMG/FSH-hCG. hMG, human menopausal gonadotropin; FSH, follicle-stimulating hormone; hCG, human chorionic gonadotropin.
Fig. 1. Ovulation induction with hMG/FSH-hCG. hMG, human menopausal gonadotropin; FSH, follicle-stimulating hormone; hCG, human chorionic gonadotropin. Fig. 2. Low-dose ovulation induction with FSH for polycystic ovaries.
Fig. 2. Low-dose ovulation induction with FSH for polycystic ovaries. Fig. 3. Informed consent for the use of hMG/FSH.
Fig. 3. Informed consent for the use of hMG/FSH. Fig. 4. Informed consent for the use of human chorionic gonadotropin.
Fig. 4. Informed consent for the use of human chorionic gonadotropin.