INTRODUCTION
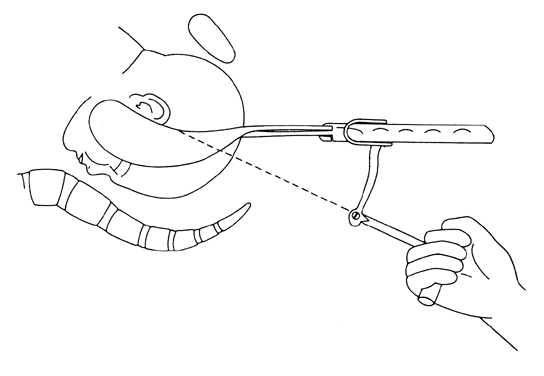
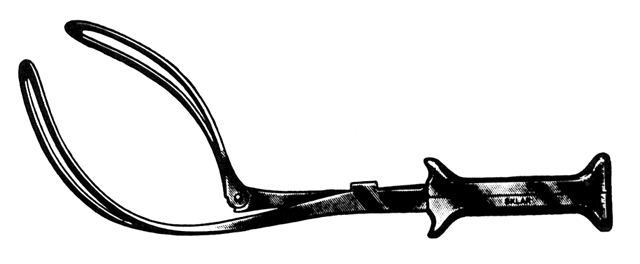
The era of modern operative obstetrics began with the invention of the forceps (Fig. 1) by Peter Chamberlen, Sr. Subsequently, over the years the ability to use forceps separated the obstetricians from the midwives. The use of forceps reached its acme in the United States as a result of the influence of DeLee, who in 1920 taught the importance of prophylactic forceps and episiotomy to protect against maternal and fetal injury.
|
|
Dennen1 emphasized the importance of knowledge about and training in the use of forceps:
“Detailed instruction in the use of the various types of obstetrical forceps is difficult to obtain. . . . A thorough knowledge of the advantages and disadvantages of the various types of forceps, and the techniques of their use will eliminate many of the bad results following blind faith in one type, or the ‘trial and error method’. . . . A properly chosen and well-executed forceps delivery does not increase the risk of a bad result. Nor does the operator, in the average case, have to be one of exceptional skill, provided he has had detailed training in the use of forceps and knows his limitations.”
DeLee’s teaching was the impetus for the dramatic increase in the number of forceps deliveries performed in the United States from the 1930s through the 1950s. However, due to the provocative studies by Friedman and colleagues2, 3, 4 and the increasing tendency for an adverse obstetric outcome to result in a malpractice suit, obstetric forceps delivery rates have fallen in the United States. In 1968 in New York City, 29.7% of births were forceps assisted, but by 1978 the incidence was down to 12.2%.5
At the same time, in the United States, cesarean birth rates rose from 5.5% in 1970 to 15.2% in 19785 and now is as high as 20–25%.
In an attempt to evaluate the diminishing opportunity for trainee obstetricians to develop skills and knowledge in the techniques of midforceps delivery, Healy and Laufe6 sent questionnaires to 144 US and Canadian members of the Association of Professors of Obstetrics and Gynecology to survey residency training in the use of forceps. They analyzed 105 programs delivering approximately 283,000 women in 1981. All programs used outlet forceps, and all but one used midforceps.
Significantly, staff obstetricians were present and instructing in the delivery room only 50% of the time in the United States, but in Canada a staff obstetrician was the principal instructor. Further, the mode of selection of the forceps most commonly used for midforceps and outlet forceps was habit and past experience, rather than design and function.
Ironically, the authors of the study pointed out, two major postgraduate obstetrics texts devoted fewer than 2% of their pages to forceps delivery. Ramin and associates7 surveyed 295 US and Canadian residency programs; of these, 203 responded, representing 458,000 deliveries with results similar to those of Healy and Laufe.6
They did note, however, that institutions that performed midforceps deliveries did not have a decrease in their cesarean section rates. A study by Powell et al.8 in 2007 found that current training results in a substantial portion of residents graduating who do not feel competent to perform forceps deliveries and this affected their future operative delivery plans. Dennen1 emphasized detailed lectures about forceps, practice with mannequins, and supervision first in easy cases and later in more complicated ones to ensure proper training in the use of forceps.
A vicious cycle of decreased opportunity, poorly supervised procedures, and even lack of detailed instruction in textbooks may lead to a generation of obstetricians who are lacking skills in forceps deliveries and therefore are unable to pass these skills on to the next generation.
Is the abandonment of forceps (especially midforceps) deliveries desirable? The issue is clearly debated in two articles, one by Friedman, who is against it,9 and the other by Hayashi, who is for it.10 Interestingly, both authorities quote many of the same articles to support their opposing points of view.
Friedman makes a compelling argument for abandoning midforceps by proposing that failure to prove statistical significance for poor outcomes is not the same as proving that a significant difference does not exist. In contrast, Hayashi made the following statement: “Although the controversy surrounding midforceps deliveries is real, it appears that the bulk of the evidence would support the use of this technique when properly indicated and skillfully applied in the management of labor.”10
While there is little controversy about the use of low or outlet forceps, which are accepted as safe methods for expediting delivery, a major controversy exists over the safety of midforceps operations for both fetus and mother. The problem with studies of midforceps operation has always been and will continue to be one of determining whether the operation really is a midforceps one. In an effort to simplify the terminology for forceps procedures and redefine midforceps, the American College of Obstetricians and Gynecologists (ACOG) reclassified forceps deliveries according to station and rotation (Table 1).11
Table 1. Classification of forceps deliveries according to station and rotation
| Type of procedure | Criteria |
| Outlet forceps | 1. Scalp is visible at the introitus without separating labia |
| 2. Fetal skull has reached pelvic floor | |
| 3. Sagittal suture is in anteroposterior diameter or right or left occiput anterior or posterior position | |
| 4. Fetal head is at or on perineum | |
| 5. Rotation does not exceed 45° | |
| Low forceps | Leading point of fetal skull is at station |
| a. Rotation |
|
| b. Rotation >45° | |
| Midforceps | Station above +2 cm but head engaged |
| High | Not included in classification |
(American College of Obstetricians and Gynecologists. Operative Vaginal Deliveries. Technical Bulletin No. 196, ACOG, Washington, DC 1994)
The reasons for forceps applications may be fetal or maternal. Forceps can be used to correct rotational defects or abnormalities of fetal attitude (deflexions). Often, the two conditions go together and are corrected with appropriate forceps maneuvers. Forceps can also be used to aid maternal expulsive efforts, which may be impeded by exhaustion, sedation, or regional anesthetics.
Forceps can be used to expedite deliveries in cases of fetal or maternal needs. A prolonged second stage of labor with prolonged compression of the pelvic floor may cause damage to the pelvic muscular supports and nerves to the pelvic muscles. This damage may be a cause of later difficulties with continence of urine and stool. The proper use of forceps to shorten the prolonged second stage of labor may prevent these long-term disabilities. Forceps should not be used to overcome cephalopelvic disproportions.
Schifrin12 criticized ACOG for making new definitions and changes in forceps delivery classification without support from conclusive data. Hagadorn-Freathy and co-workers,13 however, prospectively studied 357 forceps deliveries, comparing the older classification with the newly recommended classification. Allowing a 45° rotation or less at S + 2 or more did not increase morbidity measured by any criterion.
In evaluating midforceps procedures as currently defined, they did find increased morbidity; however, they pointed out that outcomes may reflect the experience of the institution where the study is performed.
Schifrin12 questioned whether the redefinition provides better tabulation of actual practice and really comes through in its promise to diminish the risks of forceps deliveries for mothers and babies. He also indicated that the new classification provides no new data for evaluating the specific impact of midforceps procedures on the prosecution and defense of malpractice litigation. Schifrin correctly pointed out numerous confounding variables that make evaluation of forceps data virtually impossible (Table 2).
Table 2. Evaluation of forceps data
| Confounding variables | |
| Fetus | Anesthesia |
| Estimated weight | Type |
| Actual weight | Dosage |
| FHR pattern | Timing |
| Fetal Head | Efficacy |
| Engagement | Clinical |
| Station | Parity |
| Position | Maternal weight/height |
| Attitude | Indication |
| Molding | Previous pregnancy outcome |
| Synclytism | Accuracy |
| Pelvis | Experience |
| Type | Skill |
| Dimensions | Intention |
| Forceps | Outcome |
| Type | Apgar score, pH/hypoxia |
| Rotation | Trauma |
| Force | Seizures |
| Number of attempts | Handicap |
| Labor | Disability |
| Duration | Anomaly |
| Pattern | |
| Contractions | |
| Pushing | |
FHR, fetal heart rate.
(Schifrin BS: Polemics in perinatology: disengaging forceps. J Perinatol 8(3):242, 1988)
I believe Schifrin has correctly identified the problem with classifying any forceps operation. It is quite clear that estimating fetal weight is fraught with error, leading to miscalculations in the difficulty of delivery. Neither clinical experience nor the use of ultrasound seem to have improved estimations of fetal weight. The accurate estimation of the station of the fetal head is probably the most common problem in evaluating a forceps operation. Difficulties with determining position and attitude become complicated by molding and asynclitism. Determining the midstation of the pelvis and defining the station are difficult for less experienced operators.
Although the type of pelvis and its dimensions are important in determining the type of forceps and the delivery technique, rarely is this calculated by inexperienced operators. The forceps used should be chosen for their designed function. There are numerous types of forceps, each offering distinct advantages, while others are designed for specific functions. When describing a forceps operation, how can one describe the amount of force utilized? How can one describe the accuracy of the rotational movements of the instruments? How much help can the woman give with her bearing-down efforts? How much of the efforts have been obtunded by the effects of the anesthesia used? How can we compare the outcomes of fetal distress in the second stage of labor delivered by midforceps compared to cesarean section?
Finally, how do we assess whether the outcome was the result of delivery technique or preexisting circumstances?
Schifrin appropriately makes the following generalizations:
- Delivery is not a major determinant of neurobehavioral outcome.
- Compared to spontaneous delivery, midforceps carry an increased risk of trauma and neurobehavioral abnormalities.
- Meticulous technique, limited to carefully selected, clearly indicated cases should minimize the potential for maternal/fetal damage. Under these conditions, presumably, midforceps operations may be as safe or safer for both mother and offspring than cesarean sections. Comparisons between deliveries by midforceps with deliveries by cesarean section, when controlled for indication (distress, dysfunctional labor, etc.) fail to support a significant benefit for either.
- The classification of the forceps procedure is less important than the deliberations on how carefully the case is selected.
- The medically indicated use of forceps does not present prima facie evidence of malpractice.
- A detailed discussion of the indications, intentions and technique must be included in the operative note and discussed with the patient beforehand.12
To fulfill these precepts, detailed instruction and supervision of forceps operations by experienced teachers must once more become part of any complete training program in obstetrics. A successful forceps operation does not depend on the technical skill of the operator, but on the operator’s judgment and experience.
Schifrin12 espoused the concept that defense against litigation requires a reasonable note, which should contain the indication for the forceps, a statement of informed consent, the station of the vertex, the attitude, degree of flexion, the instrument chosen, and the effort needed to complete the operation. Apgar scores, cord blood gases, and a description of any trauma observed should be recorded. These notations, clearly stated at the time of delivery, are the obstetrician’s best defense in the event of litigation.
ANATOMY OF THE FORCEPS
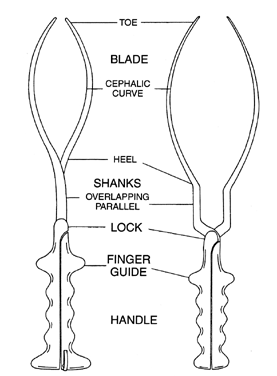
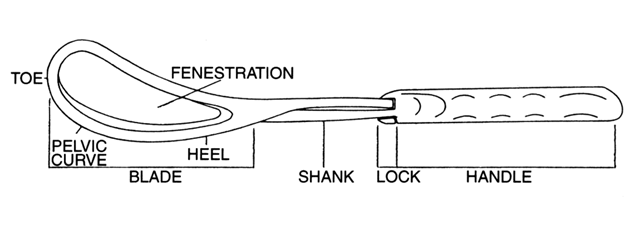
The forceps consists of a blade connected to a handle by a shank (Fig. 2 and Fig. 3). The blade may be fenestrated or solid and has two curves: the cephalic curve to encompass and protect the fetal head, and a pelvic curve to accommodate to the maternal pelvic curve. The tip of the blade is called the toe, and the back of the blade is called the heel. The shanks may be overlapping (Elliot-type forceps) or parallel (Simpson-type forceps). The shanks meet at a fulcrum point, where a lock joins them (Fig. 4).
There are several lock configurations, but the most common are the English and sliding locks. The handle is used for gripping the forceps. It should be noted that each feature of a forceps was designed for a purpose, and knowledge of the reasons for these features is important for the proper use of the forceps. Fenestrated blades allow the infant’s cheeks to bulge through and prevent slippage on the baby’s face; however, since present-day forceps procedures should not require excessive force, fenestration is not needed. Further, fenestrated blades tend to leave bruise marks more readily than solid blades.
There are two types of solid blades: (1) smooth, as seen in the Tucker-McLane modifications of the Elliot forceps (Fig. 5); and (2) pseudofenestrated, devised by Luikart and Garrison. Overlapping shanks, as seen in the Elliot or Tucker-McLane forceps, are accompanied by more space toward the heel of the blades. This makes these forceps more favorable for delivery of an infant with an unmolded head. The overlapping shanks also cause less stretching of the perineum and are therefore a better choice for rotation maneuvers. The parallel shank and longer blade make the Simpson-type forceps more appropriate for delivery when molding and caput are present. The sliding lock of the Kielland and Barton forceps helps correct asynclitism.
|
|
|
|
The two basic types of “classic forceps” are the Elliot type and its modifications and the Simpson type and its modifications. Other forceps designed for specific functions, namely the Kielland, Barton, and Piper forceps, are discussed subsequently.
PREREQUISITES FOR FORCEPS DELIVERY
It is extremely important that the prerequisites for forceps delivery be met before the procedure is attempted:
- The head should be engaged and the station of the head accurately known. In a complicated case where there is a question of whether the head is well into the pelvis, it is helpful to do a rectal examination and verify whether the head fills the sacral hollow. If the level of the head is high, it will not fill the hollow of the sacrum and a reevaluation regarding the advisability of proceeding is justified.
- The cervix should be completely dilated.
- The exact position of the head should be known. Occasionally ultrasound may help if the degree of molding creates confusion.
- The type of pelvis should be known. Certain pelvic types will not allow for rotation. For example, a fetus in a posterior position in an android or anthropoid pelvis is best delivered in the occipitoposterior (OP) position.
- The operator should be familiar with the advantages and disadvantages of the different types of instruments and their use.
- There should be adequate anesthesia for the magnitude of the forceps delivery contemplated. A low or outlet forceps delivery can be performed under pudendal block anesthesia; however, a forceps rotation of greater than 45° or a midforceps procedure requires a good epidural, saddle block, or general anesthesia.
- The bladder should be empty.
- This is an operative procedure, and it should be accorded the same respect and care for aseptic technique as any other operative procedure.
APPLICATIONS
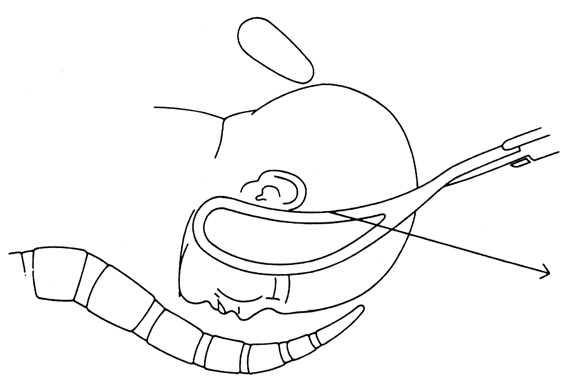
All applications of the forceps must be cephalic. That is, the forceps must be applied so they fit the head accurately. They should lie evenly against the sides of the head, reaching from the parietal bones to and beyond the malar eminences covering symmetrically the spaces between the orbits and the ears (Fig. 6).
There are three landmarks to be considered in checking the diagnoses of a proper forceps application: (1) the posterior fontanelle, (2) the sagittal suture, and (3) the fenestration. The posterior fontanelle in anterior positions should be one finger breadth above the plane of the shanks.
If the relationship of the plane of the shanks to the posterior fontanelle is not proper, the pivot point of the head will not be in the center of the widest diameter of the cephalic curve of the blades, and traction may cause either overextension or overflexion of the head, resulting in larger diameters passing through the birth canal and increasing the risk of trauma to the maternal soft tissues.
The sagittal suture should be perpendicular to the plane of the shanks. Failure to make this observation can lead to a brow-mastoid application with the risk of trauma to the infant’s facial nerve or eye.
Finally, the posterior fenestration of the blade should admit no more than a fingertip. In solid-blade forceps, this must be estimated. If there is too much room at the heel of the blades, they may not be anchored at or below the malar eminences, and traction may cause slippage and cutting of the infant’s face.Technique of forceps application
With the criteria for forceps application met, the forceps can be applied. The operator stands before the perineum with the forceps articulated and oriented to the position of the fetus’ head. Holding the forceps articulated prevents confusion due to the crossing of the shanks.
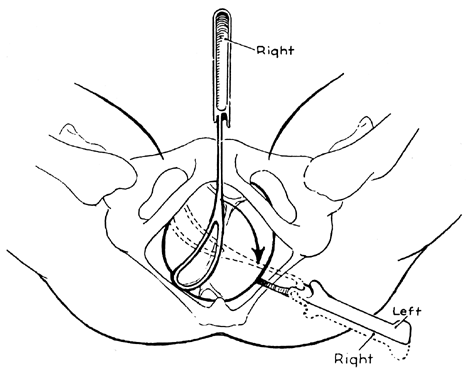
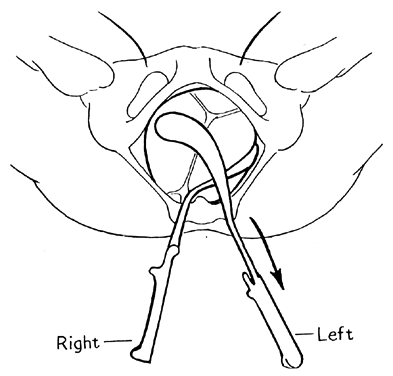
For the left occipito anterior (LOA) or direct OA positions, the left blade (posterior) is applied first. Applying the left blade first has the advantage of not needing to cross the shanks in order to lock the forceps (see Fig. 4). The operator places his or her back to the maternal right thigh and holds the handle between the fingers, as in holding a pencil. The shank is held perpendicular to the floor, the middle and index fingers are inserted into the vagina, and the thumb is applied to the heel of the blade (Fig. 7).
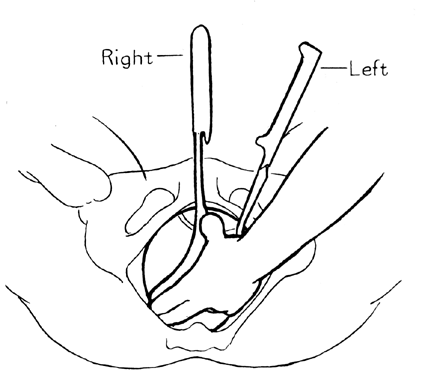
The force necessary to insert the blade is exerted by the pressure of the thumb. The left hand guides the handle in a wide arc until the blade is in place. This blade is then held in place by an assistant. The right blade is then inserted in a similar manner, with the operator’s back to the patient’s left thigh. This blade is inserted more anteriorly in the vagina to avoid rotating the head further to the left (Fig. 8).
Any adjustments to ensure a cephalic application should generally be made with the right blade. Once the blades are applied, the accuracy of placement should be evaluated. Is the occipital fontanelle one finger breadth above the shanks of the forceps? Are the shanks perpendicular to the sagittal suture? Is there only a fingertip or less space at the heel of the blade?
|
|
|
|
For the LOA position, the handles are now swept in a wide arc counterclockwise to bring the head into the OA position (Fig. 9). For the ROA position, the handles are rotated clockwise. It is important that the handles be rotated in a wide arc; unless this is done, the toes of the blades, because of the pelvic curve, will be rotated through a wide angle in the vagina, increasing the risk of maternal trauma (Fig. 10).
Once the forceps has been applied and rotation to an OA position accomplished, traction is to be applied. The operator should be seated in front of the patient, with elbows kept pressed against the sides of the body. To avoid excessive force during traction, the only force exerted should be that which can be exerted only through the wrist and forearms. The Pajot-Saxtorph maneuver provides the best grip for exerting traction (Fig. 11).
The left hand grips the shanks and exerts a downward pull. The right hand grips the handles and exerts a pull parallel to the floor. The force exerted in each direction will determine the vector of the force (Fig. 12).
|
|
An alternative method of traction is to use a Bill axis traction handle and pull in the direction of the pointer (Fig. 13). In exerting traction, it is well to keep in mind the bell-shaped curve of a uterine contraction as seen on a fetal monitor. The traction force should gradually increase, reaching its acme at about 30–40 seconds and then gradually relaxing.
For the resident being taught, it is instructive to actually count off the seconds out loud so that they can appreciate the time involved. Between tractions, the handles are unlocked to relieve pressure on the fetus’ head. The amount of force applied and the vector of pull to advance the head will vary, and adjustments will be made as the operator gains experience. When the occiput comes under the symphysis, the head can be gently extended with one hand on the forceps handles.
When the extension is almost complete, the forceps can be removed, right blade first and left blade second, and the delivery completed by the Ritgen maneuver (Fig. 14).
|
|
|
|
The question of when to perform an episiotomy in conjunction with forceps delivery is debatable. The advantages and disadvantages of an episiotomy are beyond the scope of this chapter and are discussed elsewhere. However, I prefer to perform the episiotomy before applying the forceps.
Although this may entail a slightly increased blood loss, it does allow more room for inserting the fingers and forceps. An alternative method is to apply the forceps and, before the perineum is stretched too greatly, to perform the episiotomy.
For low forceps or midforceps from the occipitotransverse (OT) positions using the classic instruments, the above-mentioned techniques apply. However, flexion of the head should be accomplished and maintained. The wide sweep of the handles for the rotation is vital for the prevention of injury to the mother (see Fig. 10).
Occipitoposterior positions
Since a persistent OP position is usually accompanied by a degree of deflexion, a bigger diameter is presented to the maternal pelvis. Therefore, it is preferable to perform a forceps maneuver that will flex and rotate the head for delivery. If a classic instrument is chosen, the Scanzoni or modified Scanzoni maneuver may be chosen.
The original Scanzoni maneuver consisted of applying the forceps as though the occiput were anterior (i.e., LOP is considered an ROA), rotating the head to the OA position and reapplying the forceps again to achieve delivery. The modified Scanzoni maneuver is more likely to succeed in converting a posterior to an anterior position, but the operator should be aware that delivery in the posterior position may be more desirable in a patient with an anthropoid or android pelvis.
In this maneuver, the forceps most appropriate is a Tucker-McLane or Elliot-type forceps with a solid blade. The forceps are applied as though to an anterior position, and after flexing the head, a wide sweep of the handles rotates the head to an OA position. The forceps are now upside down and cannot be used for delivery. The anterior blade is now removed, leaving the posterior blade splinting the head and preventing its rotating back to its original position. The anterior blade is now inserted against the head inside of the posterior blade, the posterior blade is removed and reinserted as the anterior blade, and delivery can be accomplished (Fig. 15, Fig. 16, Fig. 17, Fig. 18, Fig. 19, and Fig. 20).
One caveat: often arrest of the fetal head occurs at the tightest part of the pelvis, so that rotation may be facilitated at a higher plane by dislodging the head upward with the forceps before rotation. A solid blade is preferred because with a fenestrated blade, one blade may pass through the other during this maneuver and become entangled, causing technical problems with the delivery.
|
|
SPECIAL INSTRUMENTS
Over the years, special forceps have been created to overcome specific problems. Three of these instruments are of note: (1) Kielland forceps, (2) Barton forceps, and (3) Piper forceps.
Kielland forceps
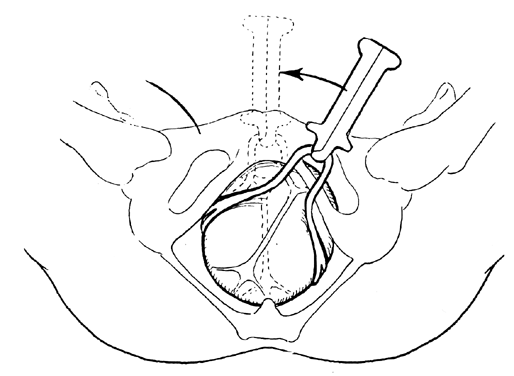
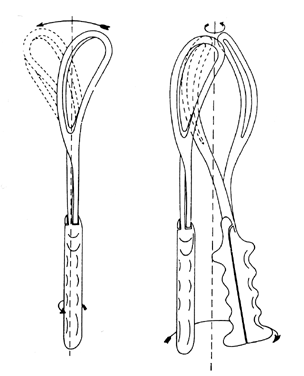
The Kielland forceps were introduced in 1915 by Dr Christian Kielland, and this instrument has several significant modifications from the classic forceps. The blades have only a slight pelvic curve, the shanks are overlapping and joined by a sliding lock, and knobs on the finger grips identify the anterior surface of the instrument. The Kielland forceps are excellent for correcting most rotational defects because of the minimal pelvic curve of the blades, enabling the operator to rotate the forceps like turning a key in a lock (Fig. 21).
The technique of application of the forceps depends on the position of the fetus’ head. For direct OP, ROP (7 o’clock), or LOP (5 o’clock) a direct application is performed. It is important before applying the forceps, to hold them articulated with the knobs facing the occiput. Once again, it is important to emphasize that since the head may be arrested at a tight portion of the pelvis, it may be necessary to either elevate or bring the head down a little before exerting a rotational effort. Since there is little pelvic curve, the handles can be turned in the appropriate direction like turning a key in a lock.
In addition, due to the lack of a pelvic curve, the direction of pull is in the plane of the pelvic curve. Once the head reaches the pelvic floor and extension is to occur, it is important to remember that the handles should not be elevated above the horizontal. This is because, due to the lack of a pelvic curve, elevating the handles above the horizontal will dig the toes of the blades into the vagina increasing the risk of sulcus tears. This can be overcome by opening the forceps, lowering the handles, reapproximating, and continuing the extension until the head is delivered or deliverable via the Ritgen maneuver.
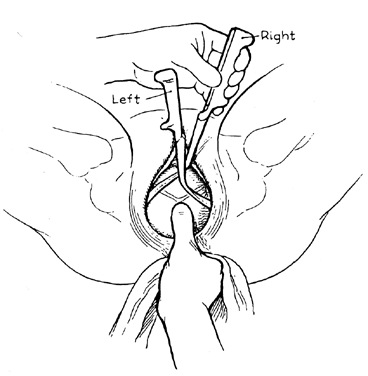
For the more transverse positions (see Fig. 8, Fig. 9, and Fig. 10; or Fig. 2, Fig. 3, and Fig. 4), two options are available: (1) classic application or (2) the direct application (Fig. 22). In the classic application, the forceps are articulated and the knobs face the occiput. The anterior blade is always applied first. For the LOT position, the right (anterior) blade is inserted first. The forceps is held in the operator’s right hand.
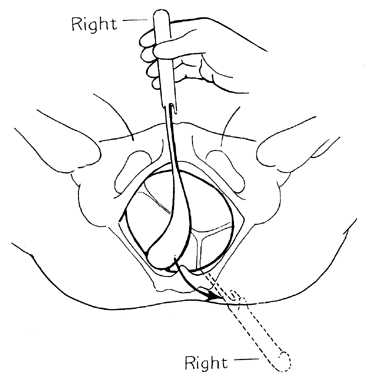
The left hand guides the toe of the blade past the cervix (Fig. 23A). At the beginning of the insertion, the shanks are at a 45° angle above the horizontal. As the blade enters the uterus, there is usually a little gush of amniotic fluid as the uterine wall is elevated from the fetus’ head. When the blade is entirely inside the uterus, the shanks are parallel to the horizontal. At this time the thumb is pressed against the fingerguard counterclockwise (Fig. 23B), causing the forceps blade to rotate to bring the cephalic curve over the fetus’ face (Fig. 23C).
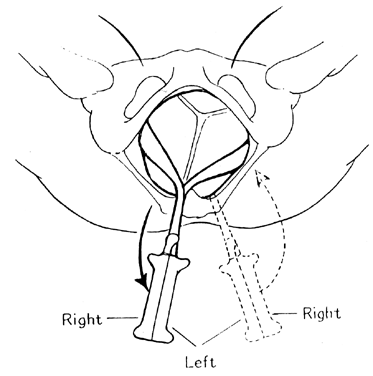
The left blade (posterior) is now inserted directly. It is important that this blade be inserted to the right side of the anterior blade, since crossing of the shanks would be dangerous. The operator’s left hand should be deep in the vagina, guiding the toe of the blade alongside the head and passing by the sacral promontory (Fig. 23D). The shanks are then articulated. The advantage of the sliding lock now become apparent. Since most OT positions involve some degree of asynclitism, pulling down on the fingerguard of the forceps blade closest to the perineum will correct the asynclitism. With the forceps properly articulated, rotation (Fig. 23E) and then extraction (Fig. 23F) can occur.
For the ROT position, the same maneuvers are performed, except that the left blade is the anterior blade inserted with the right hand and the right blade is the posterior blade. Alternative to the classic application, a direct application may be employed.
|
|
|
|
Barton forceps
The Kielland forceps, despite its versatility as a rotating forceps, cannot be used when there is a deep transverse arrest in a platypelloid pelvis. This is because the fetus must be delivered in the OT position and the cephalic curve of the anterior blade of the Kielland forceps would be forced against the symphysis, potentially damaging the symphysis or the bladder.
To resolve this problem, in 1925 Dr Lyman Barton introduced the Barton forceps. Special features of the Barton forceps (Fig. 24) are an anterior hinged blade, flexible over an arc of 90°, and a posterior blade with a deep cephalic curve. The blades are attached to the shanks at an angle of 50°, forming a perfect pelvic curve when held with the shanks perpendicular to the horizontal.
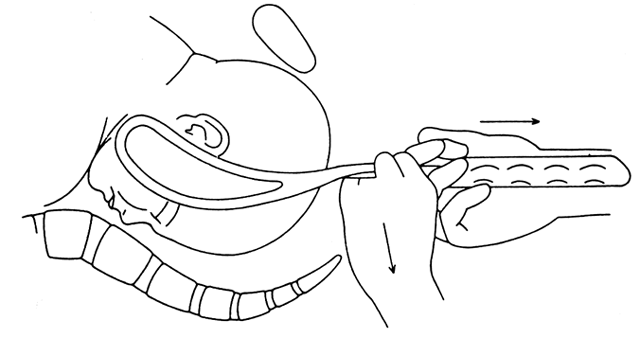
The anterior hinged blade is always inserted according to the wandering technique. When the vertex is flexed, the insertion is over the occiput. When the vertex is deflexed, the insertion is over the face. Properly positioned, the hinge should be close to the sagittal suture and one fingerbreadth medial to the occiput. The posterior blade is then inserted, with care being taken to ensure that the blade will fit into the sliding lock.
The guiding fingers should be high in the pelvis to ensure that the tip of the blade passes the sacral promontory. The anterior hinged blade is then articulated to the sliding lock. A Bill axis traction handle can then be applied, and with gentle but firm traction, the head is brought down in the OT position until it crowns under the pubic arch. At this time, rotation to the OA position can be performed by rotating the forceps handles.
In the absence of a Bill handle, a towel can be wrapped around the forceps shanks and used as a traction handle, or Pajot-Saxtorph’s maneuver can be used. Although the Barton forceps can be used for other types of rotations, its most important use is for delivery of OT positions in a platypelloid pelvis.
Piper forceps
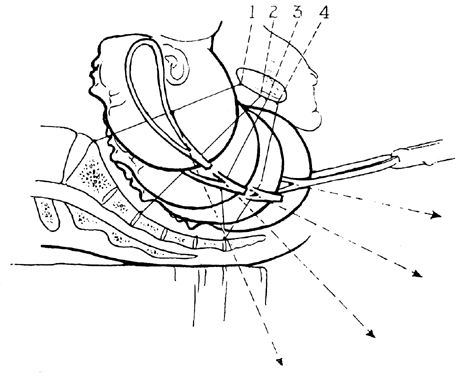
Introduced by Dr Edmund B. Piper in 1924, the Piper forceps was designed to facilitate delivery of the aftercoming fetal head in breech deliveries. Piper forceps should be on the table, unwrapped, and ready for use in any attempted vaginal breech delivery. Piper forceps (Fig. 25) are characterized by long shanks with a backward curve dropping the handles well below the level of the blades.
The dropped handles allow direct application to the baby’s head without the necessity of elevating the body above the horizontal. The backward bend also gives axis traction. The blades have no pelvic curve, allowing direct application to a high head.
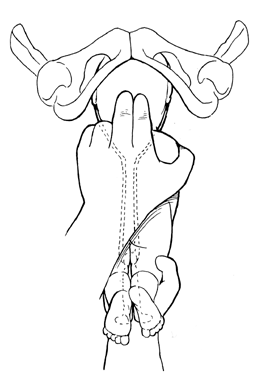
If the Mauriceau-Smellie-Veit maneuver or its modifications fail to deliver the head easily, Piper forceps should be promptly applied. Excessive traction on the body may lead to a high and severe spinal cord injury due to subluxation of the atlas on the axis. The infant should be supported by an assistant, and the operator should kneel for the forceps insertion. The left blade is applied directly to the right side of the baby’s face. This blade is always applied first to avoid having to cross the shanks in order to lock the forceps.
The opposite blade is then applied and the forceps locked. After checking for accuracy of application, the head is delivered by downward traction. Once the face appears at the introitus, the forceps handles are elevated to flex and deliver the rest of the head. The operator’s left index and middle fingers should brace the baby’s neck and the right thumb cross over the baby’s legs to control the baby’s body during delivery (Fig. 26), delivering the head by flexion. Since the blades have no pelvic curve, a deep episiotomy should be performed to prevent damage to the vagina and perineum.
Vacuum extractions
The original vacuum extractor was designed by Sir John Young in Edinburgh in 1849. Interest in the vacuum extractor increased in Europe after Malmström developed the prototype of the modern vacuum extractor in Sweden. The Malmström extractor consisted of a metal cup with a flat plate inside it and a chain attached to the plate. The chain is placed inside a rubber tube, which is necessary to develop the vacuum, and attached to a traction bar.
Traction is applied to the cup by the chain and plate, not the rubber tubing, which is a significant improvement over previous designs. The metal cup comes in four sizes, and it is recommended that the largest cup possible be used for delivery.
There had been little enthusiasm for the vacuum extractor in the United States until 1973, when Kobayashi developed the soft Silastic cup. The Silastic cup has many advantages over the metal cup, the most important being that the vacuum can be developed quickly and therefore can be released between contractions, which decreases injury to the fetal scalp due to abrasions.
The interest in this instrument in the United States has also been stimulated by the adverse publicity that midforceps delivery has received, so much so that some obstetricians no longer perform this procedure. As an alternative, they are using the Silastic vacuum extractor rather than proceeding directly to cesarean section when the fetal head is arrested in midpelvis. The final reason for the increasing interest in this type of delivery is that some patients believe that a vacuum extractor is safer for the infant than a forceps delivery.
Theoretically, the vacuum extractor has several advantages over obstetric forceps. The “ventouse” delivery is considered by its advocates as more physiologic than forceps delivery. Only traction is applied to the instrument; therefore, if the occiput is not directly anterior, it is presumed the head will rotate at the most appropriate level in the pelvis, just as it would with a spontaneous delivery.
It is surprising how often with a vacuum extraction delivery the head rotates when it reaches the perineum. When there is loss of pelvic muscle tone due to epidural anesthesia, however, this may not occur. Also, the patient assists in the delivery; because a pudendal nerve block is satisfactory, the patient is able to push when traction is applied to the extractor, so the delivery is achieved by a combination of traction and propulsion.
There is no limit to the amount of traction that can be applied to forceps, but the vacuum extractor has been shown experimentally14 to have a 23-lb limit, which is much less than with forceps delivery and therefore considered an added safety factor. Finally, with a forceps delivery, the biparietal diameter is increased by the thickness of each forceps blade, whereas this does not occur with vacuum extraction.
Serious fetal complications have been described in infants born by Malmström vacuum extraction, including significant cranial injuries and even death.15, 16, 17 Most of these were probably due to the constant suction of the metal cup and to the use of the vacuum extractor at a high station with the cervix not completely dilated.
The modern Silastic cup, which can shape to the fetal head and has no sharp edge, causes less scalp trauma,18 and the vacuum can be built up and released between contractions with the same effect. The caput succedaneum, or “chignon,” which has to develop before the vacuum extractor can function, usually disappears within 2–3 days, and the parents should be so informed before delivery.
However, an increased incidence of cephalohematomas and retinal hemorrhages have been noted after vacuum deliveries.
For reasons listed earlier, the Silastic vacuum extractor is gaining in popularity in the United States, and several studies18, 19, 20, 21 have posed that this type of delivery is less traumatic for the mother and is as safe as a forceps delivery for the infant. In 1984, however, Nilsen22 reported on an 18-year follow-up of 62 males delivered by low forceps and midforceps and 38 delivered by vacuum extraction in Norway.
He found an actual increase in mean intelligence score in the forceps-delivered group, whereas the group delivered by vacuum extraction did not differ from the national average of those men presenting themselves for the military draft.23 Since vacuum assisted delivery is considered easier than forceps delivery, the focus of training afforded to forceps deliveries in the past has not been given to vacuum deliveries and has led to increasing numbers of complications.
Among these complications are increased risk of shoulder dystocia, postpartum hemorrhage and intracranial hemorrhage,24 and subgaleal hemorrhage.25
TECHNIQUE
As soon as the vacuum has been built up and the operator has checked that all vaginal tissue has been excluded from the Silastic cup, traction should be applied with each uterine contraction. The patient is encouraged to push at the same time so that a minimum amount of traction is required to complete the delivery. The direction of traction should be at right angles to the plane of the cup, and this requires that two fingers be inserted into the vagina to pull back the posterior vaginal wall.
With the new Silastic cups, the vacuum can be released between contractions and rapidly achieved again, thus avoiding many of the serious complications reported with the metal cup. Within six to eight pulls, it will be obvious whether the delivery will be successful; if so, approximately 20 minutes will be required to complete the delivery.
Because only traction is applied, irrespective of the position of the occiput, the fetus should rotate at the most suitable level in the pelvis, and this often happens on the perineum. The vacuum extractor mimics the normal mechanism of labor, which failed owing to the lack of expulsive efforts on the part of the uterus and patient.
Two successive detachments of the vacuum cup from the fetal head are usually considered a failure for this instrument, and a forceps delivery should then be considered. However, even if the vacuum extractor is not capable of completing the delivery, a low forceps delivery may be all that is required, and if the obstetrician does not perform mid-forceps deliveries, a cesarean section will have been avoided. With the vacuum extractor a midline episiotomy is adequate, and a pudendal nerve block is the optimal form of anesthesia.
SUMMARY
The complete obstetrician must be well trained and capable of using all of the modalities available to ensure a safe outcome for both the mother and child. It is therefore incumbent upon all obstetricians to be proficient in the knowledge and use of forceps and vacuum extractors, as well as in performing spontaneous deliveries and cesarean sections.26
Author
Allan G. Charles, MD
Chief of Obstetrics and Gynecology, Michael Reese Hospital and Medical Center, Chicago, Illinois, USA
 Fig. 1.
Fig. 1.