Bill Gates taking the Ice Bucket Challenge / Image Credit: The Gates Notes
In 2014, social media was abuzz with viral videos from users of the ALS Ice Bucket Challenge. The challenge required that people pour ice water on themselves, donate money for ALS research and challenge 3 more people to do the same. Celebrities like Lebron James, Chris Pratt, Bill Gates and many others joined the challenge and it became a worldwide phenomenon and it helped raise awareness and millions of dollars for ALS research.
The same year, the Academy Award nominated movie, The Theory of Everything, a biographical drama based on Stephen Hawking, starring Eddie Redmayne and Felicity Jones, depicted his battle with ALS, the physical and emotional struggles he faced in his gradual descent into paralysis and his battle to overcome the odds to become one of the leading minds of the 21st century.
What is ALS?
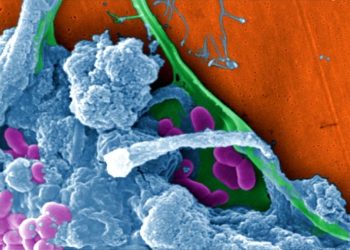
Amyotrophic Lateral Sclerosis (ALS), also called Lou Gehrig’s disease or Motor Neurone Disease (MND), is a group of rare neurological diseases that mainly involve the nerve cells (neurons) responsible for controlling voluntary muscle movement. Messages from motor neurons in the brain (called upper motor neurons) are transmitted to motor neurons in the spinal cord and to motor nuclei of the brain (called lower motor neurons) and from the spinal cord and motor nuclei of brain to a particular muscle or muscles.
Voluntary muscles produce movements like chewing, walking, and talking. The disease is progressive, meaning the symptoms get worse with time. As the motor neurons degenerate or die, they stop sending signals to muscles, start to twitch (called fasciculations), and waste away (atrophy). Eventually, the brain loses its ability to initiate and control voluntary movements.
Currently, there is no cure for ALS and no effective treatment to halt, or reverse, the progression of the disease.
Who gets ALS?
ALS is a common neuromuscular disease worldwide. It affects people of all races and ethnic backgrounds. In 2016, the Centers for Disease Control and Prevention estimated that between 14,000 – 15,000 Americans have ALS.
There are several potential risk factors for ALS including:
- Age – Although the disease can strike at any age, symptoms most commonly develop between the ages of 55 and 75.
- Gender – Men are slightly more likely than women to develop ALS. However, as we age the difference between men and women disappears.
- Race and ethnicity – Most likely to develop the disease are Caucasians and non-Hispanics.
Some studies suggest that military veterans are about 1.5 to 2 times more likely to develop ALS. Although the reason for this is unclear, possible risk factors for veterans include exposure to lead, pesticides, and other environmental toxins. ALS is recognized as a service-connected disease by the U.S. Department of Veterans Affairs.
Sporadic ALS – The majority of ALS cases (90 percent or more) are considered sporadic. This means the disease seems to occur at random with no clearly associated risk factors and no family history of the disease. Although family members of people with sporadic ALS are at an increased risk for the disease, the overall risk is very low and most will not develop ALS.
Familial (Genetic) ALS – About 5 to 10 percent of all ALS cases are familial, which means that an individual inherits the disease from his or her parents. The familial form of ALS usually only requires one parent to carry the gene responsible for the disease. Mutations in more than a dozen genes have been found to cause familial ALS. About 25 to 40 percent of all familial cases (and a small percentage of sporadic cases) are caused by a defect in a gene known as “chromosome 9 open reading frame 72,” or C9ORF72.
Interestingly, the same mutation can be associated with atrophy of frontal-temporal lobes of the brain causing frontal-temporal lobe dementia. Some individuals carrying this mutation may show signs of both motor neuron and dementia symptoms (ALS-FTD). Another 12 to 20 percent of familial cases result from mutations in the gene that provides instructions for the production of the enzyme copper-zinc superoxide dismutase 1 (SOD1).
What are the symptoms?
The onset of ALS can be so subtle that the symptoms are overlooked but gradually these symptoms develop into more obvious weakness or atrophy that may cause a physician to suspect ALS. Some of the early symptoms include:
- fasciculations (muscle twitches) in the arm, leg, shoulder, or tongue
- muscle cramps
- tight and stiff muscles (spasticity)
- muscle weakness affecting an arm, a leg, neck or diaphragm.
- slurred and nasal speech
- difficulty chewing or swallowing.
For many individuals the first sign of ALS may appear in the hand or arm as they experience difficulty with simple tasks such as buttoning a shirt, writing, or turning a key in a lock. In other cases, symptoms initially affect one of the legs, and people experience awkwardness when walking or running or they notice that they are tripping or stumbling more often.
When symptoms begin in the arms or legs, it is referred to as “limb onset” ALS. Other individuals first notice speech or swallowing problems, termed “bulbar onset” ALS.
Regardless of where the symptoms first appear, muscle weakness and atrophy spread to other parts of the body as the disease progresses. Individuals may develop problems with moving, swallowing (dysphagia), speaking or forming words (dysarthria), and breathing (dyspnea).
Although the sequence of emerging symptoms and the rate of disease progression vary from person to person, eventually individuals will not be able to stand or walk, get in or out of bed on their own, or use their hands and arms.
Individuals with ALS usually have difficulty swallowing and chewing food, which makes it hard to eat normally and increases the risk of choking. They also burn calories at a faster rate than most people without ALS. Due to these factors, people with ALS tend to lose weight rapidly and can become malnourished.
Because people with ALS usually retain their ability to perform higher mental processes such as reasoning, remembering, understanding, and problem solving, they are aware of their progressive loss of function and may become anxious and depressed.
A small percentage of individuals may experience problems with language or decision-making, and there is growing evidence that some may even develop a form of dementia over time.
Most people with ALS die from respiratory failure, usually within 3 to 5 years from when the symptoms first appear. However, about 10 percent of people with ALS survive for 10 or more years. Individuals with ALS will have difficulty breathing as the muscles of the respiratory system weaken. They eventually lose the ability to breathe on their own and must depend on a ventilator. Affected individuals also face an increased risk of pneumonia during later stages of the disease. Besides muscle cramps that may cause discomfort, some individuals with ALS may develop painful neuropathy (nerve disease or damage).
Early symptoms of ALS usually include muscle weakness or stiffness. Gradually all muscles under voluntary control are affected, and individuals lose their strength and the ability to speak, eat, move, and even breathe.
How is ALS diagnosed?
No one test can provide a definitive diagnosis of ALS. ALS is primarily diagnosed based on detailed history of the symptoms and signs observed by a physician during physical examination along with a series of tests to rule out other mimicking diseases. However, the presence of upper and lower motor neuron symptoms strongly suggests the presence of the disease.
Physicians will review an individual’s full medical history and conduct a neurologic examination at regular intervals to assess whether symptoms such as muscle weakness, atrophy of muscles, and spasticity are getting progressively worse.
ALS symptoms in the early stages of the disease can be similar to those of a wide variety of other, more treatable diseases or disorders. Appropriate tests can exclude the possibility of other conditions.
Muscle and imaging tests
Electromyography (EMG), a special recording technique that detects electrical activity of muscle fibers, can help diagnose ALS. Another common test is a nerve conduction study (NCS), which measures electrical activity of the nerves and muscles by assessing the nerve’s ability to send a signal along the nerve or to the muscle. Specific abnormalities in the NCS and EMG may suggest, for example, that the individual has a form of peripheral neuropathy (damage to peripheral nerves outside of the brain and spinal cord) or myopathy (muscle disease) rather than ALS.
A physician may also order a magnetic resonance imaging (MRI) test, a noninvasive procedure that uses a magnetic field and radio waves to produce detailed images of the brain and spinal cord. Standard MRI scans are generally normal in people with ALS. However, they can reveal other problems that may be causing the symptoms, such as a spinal cord tumor, a herniated disk in the neck that compresses the spinal cord, syringomyelia (a cyst in the spinal cord), or cervical spondylosis (abnormal wear affecting the spine in the neck).
Laboratory tests
Based on the person’s symptoms, test results, and findings from the examination, a physician may order tests on blood and urine samples to eliminate the possibility of other diseases.
Tests for other diseases and disorders
Infectious diseases such as human immunodeficiency virus (HIV), human T-cell leukemia virus (HTLV), polio, and West Nile virus can, in some cases, cause ALS-like symptoms. Neurological disorders such as multiple sclerosis, post-polio syndrome, multifocal motor neuropathy, and spinal and bulbar muscular atrophy (Kennedy’s disease) also can mimic certain features of the disease and should be considered by physicians attempting to make a diagnosis. Fasciculations and muscle cramps also occur in benign conditions.
Because of the prognosis carried by this diagnosis and the variety of diseases or disorders that can resemble ALS in the early stages of the disease, individuals may wish to obtain a second neurological opinion.
What causes ALS?
The cause of ALS is not known, and scientists do not yet know why ALS strikes some people and not others. However, evidence from scientific studies suggests that both genetics and environment play a role in the development of ALS.
Genetics
An important step toward determining ALS risk factors was made in 1993 when scientists supported by the National Institute of Neurological Disorders and Stroke (NINDS) discovered that mutations in the SOD1 gene were associated with some cases of familial ALS. Although it is still not clear how mutations in the SOD1 gene lead to motor neuron degeneration, there is increasing evidence that the gene playing a role in producing mutant SOD1 protein can become toxic.
Since then, more than a dozen additional genetic mutations have been identified, many through NINDS-supported research, and each of these gene discoveries is providing new insights into possible mechanisms of ALS.
The discovery of certain genetic mutations involved in ALS suggests that changes in the processing of RNA molecules may lead to ALS-related motor neuron degeneration. RNA molecules are one of the major macromolecules in the cell involved in directing the synthesis of specific proteins as well as gene regulation and activity.
Other gene mutations indicate defects in the natural process in which malfunctioning proteins are broken down and used to build new ones, known as protein recycling. Still others point to possible defects in the structure and shape of motor neurons, as well as increased susceptibility to environmental toxins. Overall, it is becoming increasingly clear that a number of cellular defects can lead to motor neuron degeneration in ALS.
In 2011 another important discovery was made when scientists found that a defect in the C9ORF72 gene is not only present in a significant subset of individuals with ALS but also in some people with a type of frontotemporal dementia (FTD). This observation provides evidence for genetic ties between these two neurodegenerative disorders. Most researchers now believe ALS and some forms of FTD are related disorders.
Environmental factors
In searching for the cause of ALS, researchers are also studying the impact of environmental factors. Researchers are investigating a number of possible causes such as exposure to toxic or infectious agents, viruses, physical trauma, diet, and behavioral and occupational factors.
For example, researchers have suggested that exposure to toxins during warfare, or strenuous physical activity, are possible reasons for why some veterans and athletes may be at increased risk of developing ALS.
Although there has been no consistent association between any environmental factor and the risk of developing ALS, future research may show that some factors are involved in the development or progression of the disease.
How is ALS treated?
No cure has yet been found for ALS. However, there are treatments available that can help control symptoms, prevent unnecessary complications, and make living with the disease easier.
Supportive care is best provided by multidisciplinary teams of health care professionals such as physicians; pharmacists; physical, occupational, and speech therapists; nutritionists; social workers; respiratory therapists and clinical psychologists; and home care and hospice nurses. These teams can design an individualized treatment plan and provide special equipment aimed at keeping people as mobile, comfortable, and independent as possible.
Medication
The U.S. Food and Drug Administration (FDA) has approved the drugs riluzole (Rilutek) and edaravone (Radicava) to treat ALS. Riluzole is believed to reduce damage to motor neurons by decreasing levels of glutamate, which transports messages between nerve cells and motor neurons. Clinical trials in people with ALS showed that riluzole prolongs survival by a few months, particularly in the bulbar form of the disease, but does not reverse the damage already done to motor neurons. Edaravone has been shown to slow the decline in clinical assessment of daily functioning in persons with ALS.
Physicians can also prescribe medications to help manage symptoms of ALS, including muscle cramps, stiffness, excess saliva and phlegm, and the pseudobulbar affect (involuntary or uncontrollable episodes of crying and/or laughing, or other emotional displays). Drugs also are available to help individuals with pain, depression, sleep disturbances, and constipation. Pharmacists can give advice on the proper use of medications and monitor a person’s prescriptions to avoid risks of drug interactions.
Physical therapy
Physical therapy and special equipment can enhance an individual’s independence and safety throughout the course of ALS. Gentle, low-impact aerobic exercise such as walking, swimming, and stationary bicycling can strengthen unaffected muscles, improve cardiovascular health, and help people fight fatigue and depression. Range of motion and stretching exercises can help prevent painful spasticity and shortening (contracture) of muscles.
Physical therapists can recommend exercises that provide these benefits without overworking muscles. Occupational therapists can suggest devices such as ramps, braces, walkers, and wheelchairs that help individuals conserve energy and remain mobile.
Speech therapy
People with ALS who have difficulty speaking may benefit from working with a speech therapist, who can teach adaptive strategies to speak louder and more clearly. As ALS progresses, speech therapists can help people maintain the ability to communicate. They can recommend aids such as computer-based speech synthesizers that use eye-tracking technology and can help people develop ways for responding to yes-or-no questions with their eyes or by other nonverbal means.
Some people with ALS may choose to use voice banking while they are still able to speak as a process of storing their own voice for future use in computer-based speech synthesizers. These methods and devices help people communicate when they can no longer speak or produce vocal sounds.
Nutritional support
Nutritional support is an important part of the care of people with ALS. It has been shown that individuals with ALS will get weaker if they lose weight. Nutritionists can teach individuals and caregivers how to plan and prepare small meals throughout the day that provide enough calories, fiber, and fluid and how to avoid foods that are difficult to swallow. People may begin using suction devices to remove excess fluids or saliva and prevent choking. When individuals can no longer get enough nourishment from eating, doctors may advise inserting a feeding tube into the stomach. The use of a feeding tube also reduces the risk of choking and pneumonia that can result from inhaling liquids into the lungs.
Breathing support
As the muscles responsible for breathing start to weaken, people may experience shortness of breath during physical activity and difficulty breathing at night or when lying down. Doctors may test an individual’s breathing to determine when to recommend a treatment called noninvasive ventilation (NIV). NIV refers to breathing support that is usually delivered through a mask over the nose and/or mouth. Initially, NIV may only be necessary at night. When muscles are no longer able to maintain normal oxygen and carbon dioxide levels, NIV may be used full-time. NIV improves the quality of life and prolongs survival for many people with ALS.
Because the muscles that control breathing become weak, individuals with ALS may also have trouble generating a strong cough. There are several techniques to help people increase forceful coughing, including mechanical cough assist devices and breath stacking. In breath stacking, a person takes a series of small breaths without exhaling until the lungs are full, briefly holds the breath, and then expels the air with a cough.
As the disease progresses and muscles weaken further, individuals may consider forms of mechanical ventilation (respirators) in which a machine inflates and deflates the lungs. Doctors may place a breathing tube through the mouth or may surgically create a hole at the front of the neck and insert a tube leading to the windpipe (tracheostomy). The tube is connected to a respirator.
Individuals with ALS and their families often consider several factors when deciding whether and when to use ventilation support. These devices differ in their effect on a person’s quality of life and in cost. Although ventilation support can ease problems with breathing and prolong survival, it does not affect the progression of ALS. People may choose to be fully informed about these considerations and the long-term effects of life without movement before they make decisions about ventilation support.
What research is being done?
The mission of the National Institute of Neurological Disorders and Stroke (NINDS) is to seek fundamental knowledge about the brain and nervous system and to use that knowledge to reduce the burden of neurological disease. The NINDS is a component of the National Institutes of Health (NIH), the leading supporter of biomedical research in the world.
The goals of NINDS research on ALS are to understand the cellular mechanisms involved in the development and progression of the disease, investigate the influence of genetics and other potential risk factors, identify biomarkers, and develop new and more effective treatments.
Cellular defects
Scientists are seeking to understand the mechanisms that selectively trigger motor neurons to degenerate in ALS, and to find effective approaches to halt the processes leading to cell death. Using both animal models and cell culture systems, scientists are trying to determine how and why ALS-causing gene mutations lead to the destruction of neurons. These animal models include fruit flies, zebrafish, and rodents.
Initially, genetically modified animal models focused on mutations in the SOD1 gene but more recently, models have been developed for defects in the C9ORF72, TARDP, FUS, PFN1, TUBA4A, and UBQLN2 genes. Research in these models suggests that, depending on the gene mutation, motor neuron death is caused by a variety of cellular defects, including in the processing of RNA molecules and recycling of proteins, and structural impairments of motor neurons. Increasing evidence also suggests that various types of glial support cells and inflammation cells of the nervous system may play an important role in the disease.
Stem Cells
In addition to animal models, scientists are also using innovative stem cells models to study ALS. Scientists have developed ways to take skin or blood cells from individuals with ALS and turn them into stem cells, which are capable of becoming any cell type in the body, including motor neurons and other cell types that may be involved in the disease. NINDS is supporting research on the development of stem cell lines for a number of neurodegenerative diseases, including ALS.
Familial versus sporadic ALS
Overall, the work in familial ALS is already leading to a greater understanding of the more common sporadic form of the disease. Because familial ALS and sporadic ALS show many of the same signs and symptoms, some researchers believe that some familial ALS genes may also be involved in sporadic ALS.
Clinical research studies supported by NINDS are looking into how ALS symptoms change over time in people with C9ORF72 mutations. Other NINDS-supported research studies are working to identify additional genes that may cause or put a person at risk for either familial or sporadic ALS.
Additionally, researchers are looking at the potential role of epigenetics in the development of ALS. Epigenetic changes can switch genes on and off, and thus can profoundly affect the human condition in both health and disease. These changes can occur in response to multiple factors, including external or environmental conditions and events. Although this research is still at a very exploratory stage, scientists hope that understanding epigenetics can offer new information about how ALS develops.
Biomarkers
Biomarkers are biological measures that help to identify the presence or rate of progression of a disease or the effectiveness of a therapeutic intervention. Since ALS is difficult to diagnose, biomarkers could potentially help clinicians diagnose ALS earlier and faster.
Additionally, biomarkers are needed to help predict and accurately measure disease progression and enhance clinical studies aimed at developing more effective treatments. Biomarkers can be molecules derived from a bodily fluid (such as those in the blood and cerebrospinal fluid), an image of the brain or spinal cord, or a measure of the ability of a nerve or muscle to process electrical signals. The NINDS is supporting research on the development biomarkers for ALS.
New treatment options
Potential therapies for ALS are being investigated in a range of disease models. This work involves tests of drug-like compounds, gene therapy approaches, antibodies, and cell-based therapies. For example, NINDS-supported scientists are currently investigating whether lowering levels of the SOD1 enzyme in the brain and spinal cord of individuals with SOD1 gene mutations would slow the rate of disease progression.
Other NINDS scientists are studying the use of glial-restricted progenitor cells (which have the ability to develop into other support cells) to slow disease progression and improve respiratory function. Additionally, a number of exploratory treatments are being tested in people with ALS. Investigators are optimistic that these and other basic, translational, and clinical research studies will eventually lead to new and more effective treatments for ALS.
Postscript: Ice Bucket Challenge was a remarkable success as it raised over $220 million. The ALS Association said: “Never before have been in a better position to fuel our fight against this disease. Increased awareness and unprecedented financial support will enable us to think outside the box.”